Published 01 May 2024
Macular degeneration is currently one of the leading causes of low vision and blindness in Australia, and of its various forms, Age-Related Macular Degeneration (AMD or AMRD) is the most common.
At least 1 in 7 Australians over the age of 50, or approximately 1.4 million people, have some evidence of AMD. There is no cure, but steps can be taken to slow the progression of the disease, which means that early detection through regular eye examinations is crucial to reducing the risk of vision loss in advanced stages.
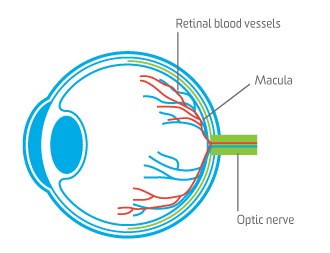
What is the macula?
The macula is a very small part of the retina at the back of the eye. It provides us with our detailed central vision, allowing us to perform tasks such as reading, driving and face recognition.
What happens when the macula is damaged?
Damage to the macula results in distorted, blurred central vision, similar to having a scratch or smudge in the centre of your glasses.
AMD has the potential to cause progressive loss of central vision, while leaving peripheral or side vision intact. This can have detrimental effects on a person’s wellbeing and quality of life as daily activities are impacted.
This chronic disease varies from person to person. It can advance slowly or quickly and can affect one or both eyes, at different rates.
While this article focuses on AMD, there are other macular diseases that can affect your vision and are important to detect early through regular eye testing. These include diabetic retinopathy, retinal vein occlusion, vitreomacular traction and myopic macular degeneration.
What are the stages of AMD?
AMD is classed into three main stages: early, intermediate, and advanced.
You can have AMD in its early stage and not have any impact to your vision, but this can still be picked up in an eye examination.
Once AMD progresses to the advanced stage it is then classified as either dry (atrophic) or wet (neovascular) and the treatments to manage each will vary.
What are the risk factors for AMD?
Three main factors increase the risk of AMD. These include:
- being over the age of 50
- having a family history of AMD
- smoking
The two strongest risk factors for AMD are beyond our control – age and family history, but the good news is that you can reduce your risk of developing advanced AMD by not smoking.
Booking in for regular eye examinations will also help make sure that AMD and other eye conditions are picked up early.
How often are eye examinations recommended?
Your optometrist will be best placed to advise how frequent your eye examinations should be, particularly if you are under 65. Their recommendation will be based on your individual circumstances such as age, general health including medications you’re taking, risk factors for eye diseases and current eye condition. It is important to communicate any family history of known eye diseases to your optometrist as this will help them evaluate your own risk level. For example, you have a 50% risk of developing AMD if a parent or sibling has the condition.
At GMHBA Eye Care, we recommend annual eye examinations once a person turns 65 years of age, and more frequent testing may be required when a specific eye condition is being monitored.
What does an eye examination involve?
Standard eye tests at GMHBA Eye Care are comprehensive and involve an optometrist consultation where they will take your detailed history, test your vision and prescription, and assess the health of your eyes.
They may recommend that you have an Optical Coherence Tomography (OCT) scan if you are at risk of having or developing AMD. The OCT scan is now considered a standard tool in the diagnosis and management of AMD and is available across all GMHBA Eye Care locations.
Find out more about getting your eyes tested.
What is an Amsler grid?
Once AMD is detected, the Amsler grid, developed by Swiss ophthalmologist Marc Amsler and used since 1945, can assist with detecting further changes to the macula. This simple take-home tool – which your optometrist can show you how to use – can help you to self-monitor your vision between eye examinations and identify any problem spots.

The images above show the standard Amsler grid on the left, and on the right-hand example, how this may appear for someone who has AMD. If you are self-testing regularly and notice any changes in how you see the Amsler grid, it is important to speak with your optometrist or ophthalmologist right away as this may indicate some changes to your macula.
What else can I do to keep my eyes healthy?
Aside from booking in for regular eye examinations, there are some key things you can do to look after your eye health.
- No smoking
Smoking triples to quadruples your risk of developing AMD, and can also bring it on earlier than non-smokers by an average of five to ten years. There is a direct association between the number of cigarettes smoked over time and the risk of developing late-stage AMD. The good news is that the eye starts to recover the moment you stop smoking, and your risk can be reduced over time, so think seriously about quitting today.
- Living a healthy lifestyle
A balanced diet rich in anti-oxidants, vitamins and minerals and staying active play an important role in supporting your eye health.
You can boost the nutrients in your diet by incorporating dark green leafy vegetables and fresh fruit daily and eating fish two to three times a week. A handful of nuts a week is also recommended.
Regular exercise is beneficial at all ages but is particularly helpful for those with low vision or at risk of low vision because it improves balance, strength, mobility, and reaction time, and can reduce the risk or impact of a fall. Read our top tips for getting more movement in your day.
- Wearing sunglasses
Not only are sunglasses a stylish choice to help reduce glare, but they also help reduce the cumulative impact of UV damage to the eye which can contribute to AMD. Find out more in our article Sunglasses – more than a fashion statement.
To find out more view the Macular Disease Foundation Australia’s Eye Health checklist.
What can I do today?
While there are no medical treatments available for early-stage macular degeneration, there is a substantial amount of research being done around the world in the hope of finding effective therapies. Following the recommended guide for reducing risk factors and keeping up with regular eye examinations is your best defence to detect and slow the progression of this disease.
The optometrists at GMHBA Eye Care can address any visual concerns you may have and will assist in finding the right support services for anyone affected with age-related macular degeneration.
GMHBA Eye Care | Book now